Why Do My Legs Feel Heavy and Tired? Understanding Venous Fatigue
Key Points
- Leg heaviness and fatigue are often the first signs of vein problems
- Venous insufficiency causes blood to pool in your legs, creating that weighted-down feeling
- Symptoms typically worsen throughout the day and improve with rest or elevation
- The heavy feeling occurs because your veins aren't efficiently returning blood to your heart
- Risk factors include prolonged standing, genetics, pregnancy, and age
- Early treatment can prevent symptoms from progressing to more serious vein disease
- Simple lifestyle changes can provide relief while you explore treatment options
That dragging, heavy sensation in your legs at the end of a long day isn't just normal tiredness. If your legs feel like you're walking through water, like they're weighted down with sandbags, or if they're so tired that climbing stairs feels like a major effort, you might be experiencing something called venous fatigue.
This isn't the kind of tired that happens after a hard workout or a day of hiking. It's different. It's a deep, achy heaviness that settles into your calves and thighs, making even simple activities feel exhausting. And here's the thing: it's one of the most common early warning signs that something isn't working right with your veins.
Let's talk about why this happens, what it means, and what you can do about it.
What Does Leg Heaviness Actually Feel Like?
Before we dive into the why, let's make sure we're talking about the same thing. Venous fatigue has some pretty distinctive characteristics that set it apart from regular muscle tiredness.
People describe the sensation in different ways:
- Like your legs are filled with lead or concrete
- A weighted-down feeling that makes your legs want to give out
- Deep achiness combined with tiredness
- Legs that feel swollen and tight, even if they don't look visibly swollen
- A dragging sensation, like your legs don't want to move
- Feeling like you need to sit down and elevate your legs just to get relief
The pattern matters too. Venous fatigue typically gets worse as the day goes on. You might feel relatively normal when you wake up in the morning, but by afternoon or evening, that heavy feeling has settled in. Standing or sitting for long periods makes it worse. Walking around sometimes helps a little, but not for long.
And here's the telltale sign: when you finally get to elevate your legs at the end of the day, you feel relief. That heavy sensation eases up, your legs feel lighter, and you can almost feel the blood draining back toward your heart where it belongs.
The Science Behind Why Your Legs Feel Heavy
So what's actually happening inside your legs to create this sensation? It all comes down to circulation and how your veins move blood back up to your heart.
Your leg veins have a tough job. They need to move blood upward against gravity, fighting that downward pull every single moment of every day. To accomplish this, your veins have tiny one-way valves that open to let blood flow up and close to prevent it from flowing backward. Your calf muscles act like a pump, squeezing the veins with each step you take and pushing blood upward through those valves.
When this system works properly, blood circulates efficiently. You don't even think about it.
But when the valves inside your veins weaken or get damaged, they can't close completely anymore. This allows blood to leak backward and pool in your lower legs. This backward flow and pooling is called venous insufficiency, and it's the root cause of that heavy, tired feeling.
Here's what happens when blood pools in your legs:
Increased pressure: The pooled blood creates extra pressure in your veins, stretching the vein walls and making them work harder. Your legs literally feel heavier because there's more blood sitting in them than there should be.
Fluid buildup: That increased pressure forces fluid out of your blood vessels and into the surrounding tissues. Even if you don't see obvious swelling, there's often subtle fluid accumulation that contributes to the heavy sensation.
Reduced oxygen delivery: When blood isn't circulating efficiently, your leg muscles and tissues don't get the fresh, oxygen-rich blood they need. This creates that deep tiredness and makes your muscles fatigue more easily.
Inflammation: Chronic blood pooling triggers low-grade inflammation in your veins and surrounding tissues, which can cause achiness and discomfort on top of the heaviness.
The longer you're on your feet or sitting in one position, the more blood accumulates in your lower legs, and the heavier they feel.
Gravity is constantly working against your veins, so symptoms build throughout the day.
Why the Heavy Feeling Gets Worse as the Day Goes On
Ever notice that your legs feel relatively okay in the morning but progressively worse by evening? There's a clear reason for this pattern.
When you sleep, you're lying flat. Your legs are at the same level as your heart, which means your veins don't have to work against gravity. Blood drains naturally back toward your heart overnight, and any fluid that accumulated in your tissues gets reabsorbed. You wake up with your circulation relatively "reset."
But the moment you stand up and start your day, gravity kicks in again. If you have weak vein valves, blood starts pooling almost immediately. Throughout the day, more and more blood accumulates in your lower legs. The pressure builds. Fluid seeps into your tissues. Your veins stretch further.
By the time evening rolls around, you've got hours of accumulated blood pooling and fluid buildup. Your legs have been fighting gravity all day long, and they're exhausted from the effort. That's why the heavy feeling is so much worse at night than it is in the morning.
This day-to-night pattern is actually a helpful diagnostic clue. If your leg heaviness is worse in the evening and better in the morning, it strongly suggests a vein problem rather than something else like a muscle or joint issue.
Who's Most Likely to Experience Venous Fatigue?
While anyone can develop venous insufficiency and experience leg heaviness, certain factors put you at higher risk.
People who stand all day: If your job keeps you on your feet for hours (teachers, nurses, retail workers, hairstylists, chefs), your calf muscle pump is working overtime, but it may not be enough to compensate for weak vein valves. Standing still is actually worse than walking because your muscles aren't actively pumping.
People who sit all day: Desk jobs present the opposite problem. When you sit for extended periods, your calf muscles aren't pumping at all. Blood pools in your lower legs with nowhere to go.
Women who've been pregnant: Pregnancy puts enormous pressure on leg veins and causes hormonal changes that can weaken vein walls. Many women first notice leg heaviness during or after pregnancy.
People with a family history: Genetics plays a major role in vein health. If your parents or grandparents had varicose veins or vein problems, you're more likely to develop them too.
Older adults: Vein valves naturally weaken with age. Years of fighting gravity take their toll, making venous insufficiency more common as you get older.
People carrying extra weight: Additional body weight puts extra pressure on leg veins, making it harder for them to move blood efficiently back to your heart.
Women taking hormonal medications: Birth control pills and hormone replacement therapy can affect vein wall strength and increase the risk of vein problems.
If you fit into one or more of these categories and you're experiencing leg heaviness, the connection to your veins is even more likely.
Other Symptoms That Often Accompany Leg Heaviness
Venous fatigue rarely shows up alone. Most people with that heavy, tired feeling in their legs notice other symptoms too. These additional signs help confirm that your circulation is the culprit.
Common companion symptoms include:
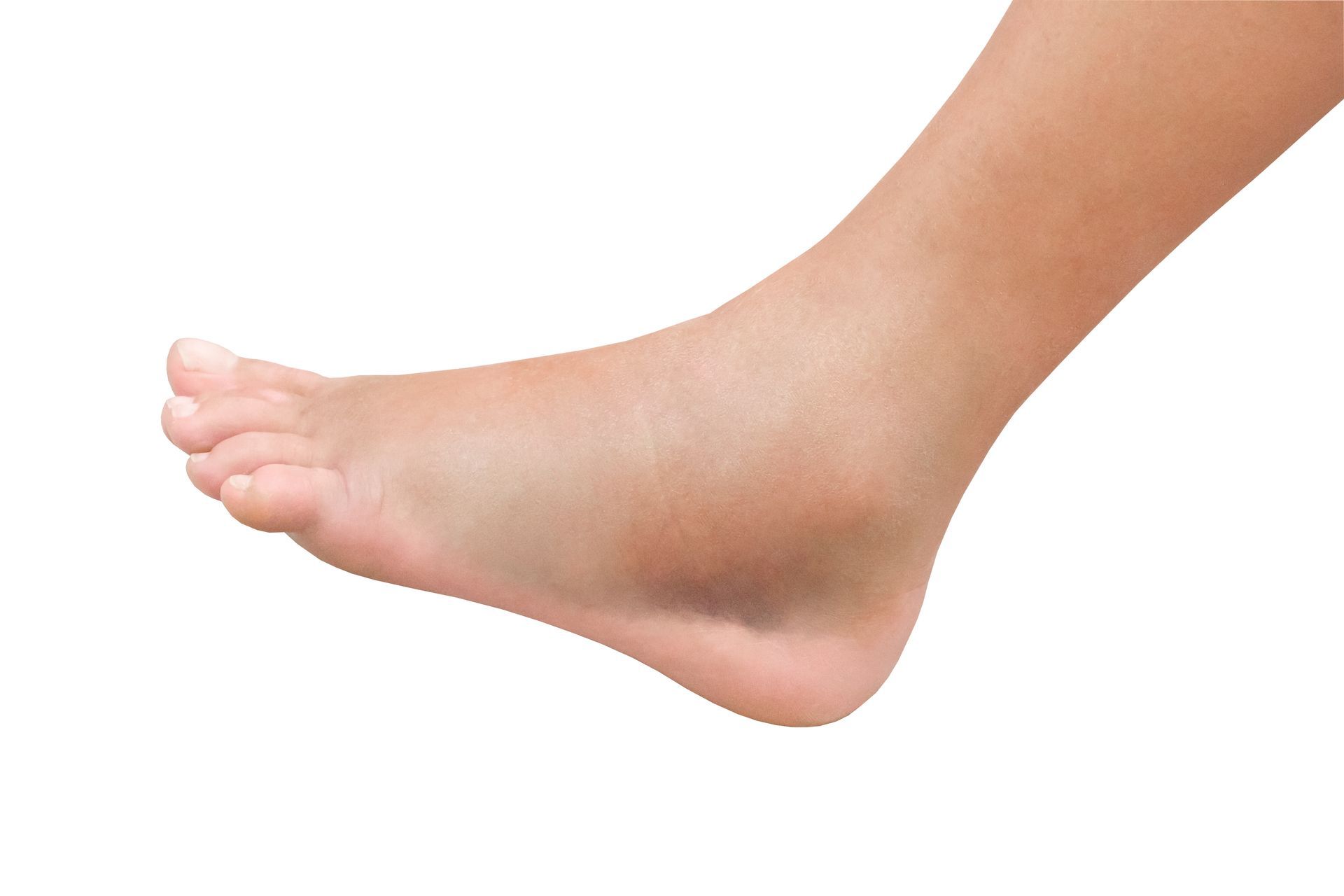
Swelling: Your ankles, feet, or lower legs may swell throughout the day. You might notice sock marks that seem deeper than they used to be, or your shoes feel tighter by evening.
Aching or throbbing: A dull, persistent ache often accompanies the heaviness. Some people describe it as a deep throb that follows the path of their veins.
Restless legs at night: Your legs might feel like they need to move when you're trying to sleep. This restlessness is your body's response to poor circulation.
Cramping: Muscle cramps, especially at night, are common when your leg circulation isn't optimal.
Itching or burning: You might experience itchy or burning sensations around your veins or on your lower legs.
Skin changes: Over time, chronic venous insufficiency can cause skin discoloration, usually brown or reddish patches around the ankles.
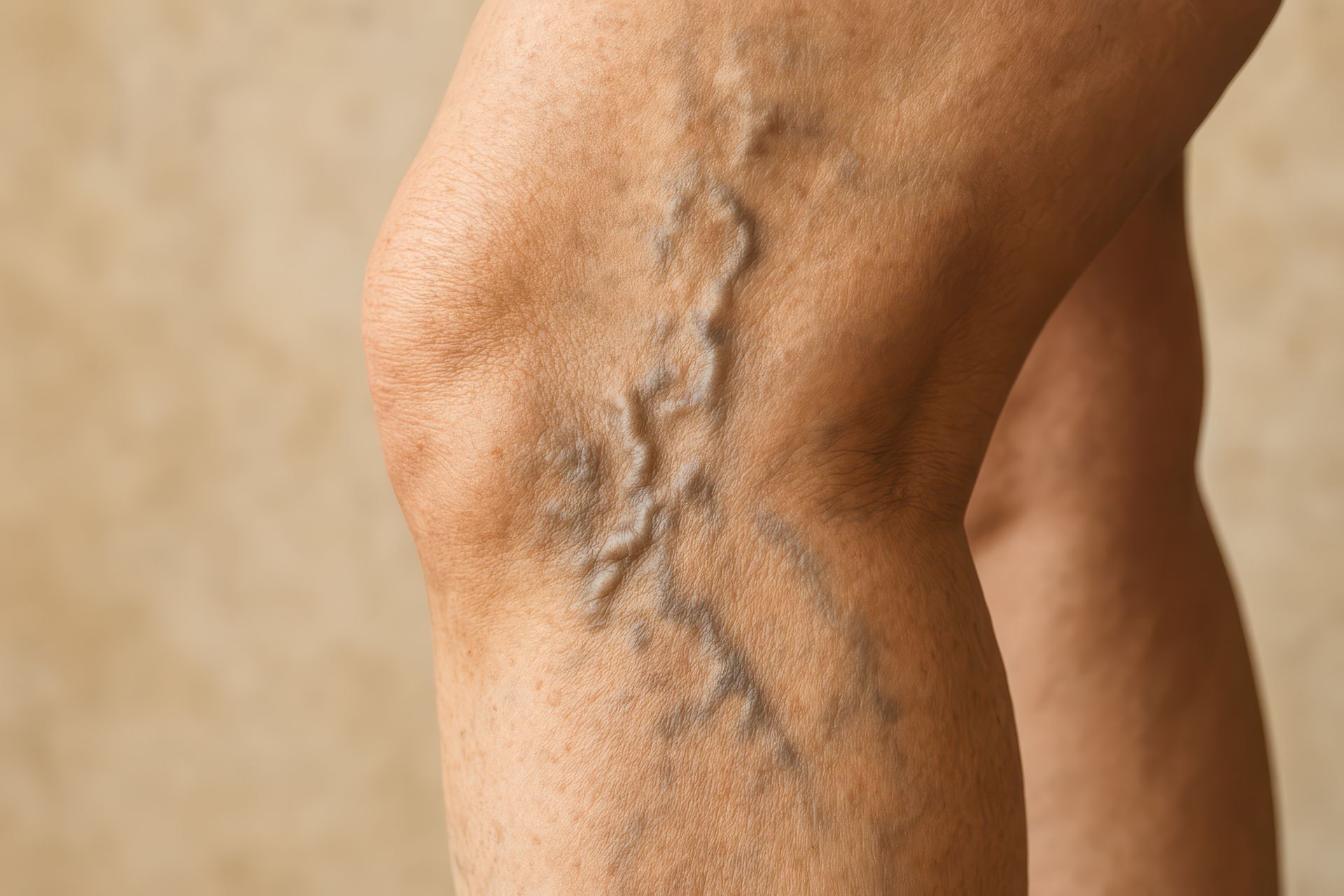
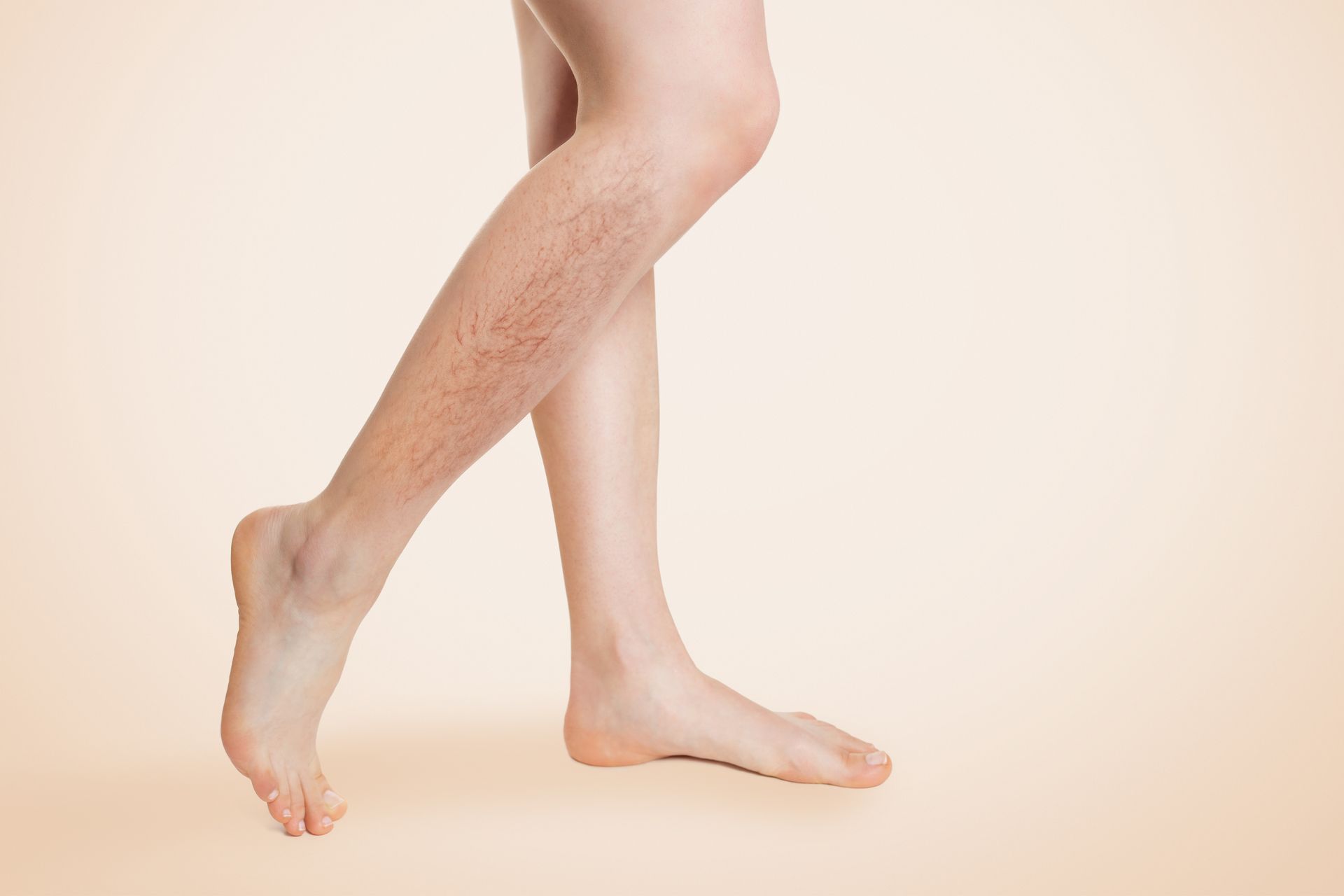
Visible veins: You may notice spider veins or bulging varicose veins appearing on your legs.
The more of these symptoms you have along with leg heaviness, the more likely it is that you're dealing with a vein problem that needs attention. To learn more about these related conditions, check out our comprehensive guide on vein problems.
When Heavy Legs Mean It's Time to See a Doctor
A little leg tiredness at the end of a long day is normal for everyone. But there's a difference between normal fatigue and venous fatigue that signals a problem.
You should consider seeing a vein specialist if:
Your symptoms are consistent and worsening: If your legs feel heavy most days, and the feeling is getting worse over time rather than staying the same, it's worth getting evaluated.
The heaviness affects your daily life: When leg fatigue limits what you can do, keeps you from activities you enjoy, or makes it difficult to get through your workday, that's a sign to seek help.
You're experiencing other vein-related symptoms: If you have leg heaviness plus swelling, visible varicose veins, skin changes, or nighttime leg issues, these combined symptoms suggest venous insufficiency.
Elevation provides significant relief: If propping your legs up dramatically improves how they feel, that's a clear sign your veins aren't circulating blood efficiently when you're upright.
You have risk factors: If you have a family history of vein problems, you've been pregnant, or you have a job that requires prolonged standing, don't ignore early symptoms. Getting evaluated early gives you more treatment options.
Conservative measures aren't helping: If you've tried compression stockings, regular exercise, and other lifestyle changes without much improvement, it's time to see what else can be done.
Dr. Michael Sorace can perform a simple, painless ultrasound evaluation to check your vein function and determine whether venous insufficiency is causing your symptoms. Early diagnosis and treatment can prevent your symptoms from progressing to more serious complications.
What You Can Do Right Now for Relief
While you're deciding whether to see a specialist or waiting for your appointment, there are several things you can do to reduce leg heaviness and improve your comfort.
Move regularly throughout the day: Set a timer to remind yourself to stand up and walk for a few minutes every hour if you have a desk job. If you stand all day, try to incorporate walking breaks or shift your weight from foot to foot to keep your calf muscles pumping.
Elevate your legs: Prop your feet up above heart level for 15-20 minutes several times a day. This gives gravity a chance to work in your favor and helps blood drain back toward your heart.
Try compression stockings: These specially designed socks provide graduated pressure that helps push blood upward. You can buy mild compression stockings at most pharmacies, or your doctor can prescribe stronger ones if needed.
Stay hydrated: Drinking plenty of water keeps your blood at the right consistency for optimal flow. Dehydration makes blood thicker and harder to pump.
Exercise your calves: Simple calf raises, ankle pumps, and walking all activate your calf muscle pump and improve circulation. Even small amounts of movement help.
Avoid crossing your legs: This position restricts blood flow and can make pooling worse.
Maintain a healthy weight: Extra pounds put additional pressure on your leg veins. Even modest weight loss can reduce symptoms.
Wear looser clothing: Tight pants, especially around the waist and thighs, can restrict circulation and contribute to blood pooling.
These strategies can provide some relief and may slow the progression of vein problems, but they won't fix damaged vein valves. Think of them as helpful management tools while you explore longer-term solutions. For more detailed tips on improving your circulation, read our post on daily habits that improve circulation and reduce vein symptoms.
What Treatment Can Do for Heavy, Tired Legs
Here's the really good news: venous fatigue responds extremely well to treatment. In fact, relief from that heavy, tired feeling is often the first and most noticeable improvement patients experience after treating their vein problems.
When you address the underlying venous insufficiency causing blood to pool in your legs, your circulation improves dramatically. Your veins can move blood efficiently again. The pressure decreases. Fluid stops accumulating. Your legs feel lighter, more energetic, and comfortable throughout the day.
Most people notice improvement within days to weeks after treatment. That constant heaviness that used to set in every afternoon? Gone. The need to prop your legs up every evening? Much less urgent. The feeling that your legs are working against you? Replaced by normal, comfortable leg function.
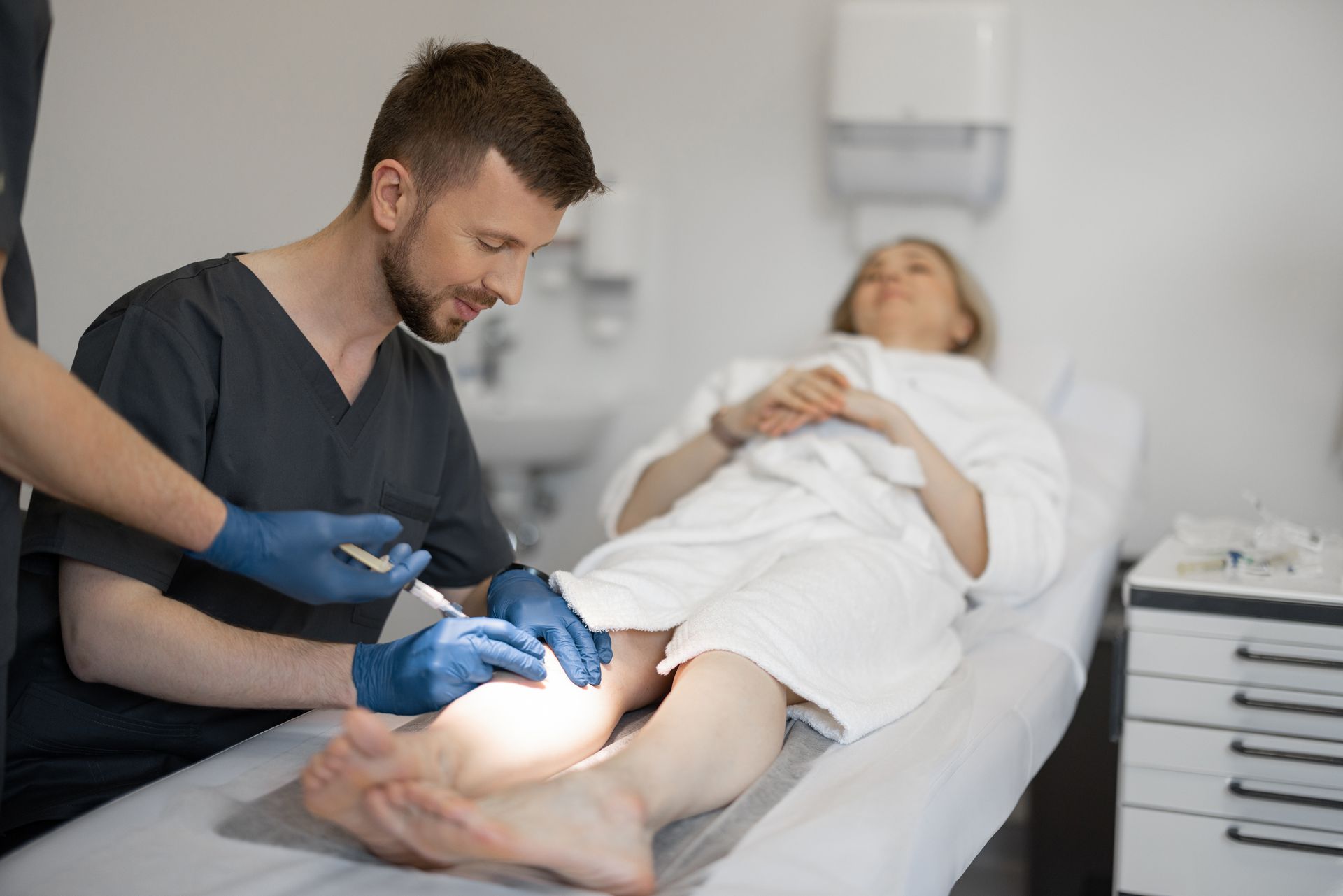
Modern vein treatments are minimally invasive and highly effective. They're performed in the office, require minimal downtime, and have excellent success rates for improving symptoms like leg heaviness and fatigue.
The Vein Institute offers comprehensive evaluation and treatment options tailored to your specific needs. The first step is understanding what's causing your symptoms and creating a personalized plan to address it.
Don't Ignore What Your Legs Are Telling You
That heavy, tired feeling in your legs isn't something you have to live with. It's not just a normal part of aging or an inevitable consequence of your job. It's your body's way of telling you that your veins need help.
Venous insufficiency is progressive, meaning it gets worse over time if left untreated. What starts as mild leg heaviness can eventually progress to more serious problems like chronic swelling, skin changes, or even venous ulcers. But here's the thing: you don't have to wait until things get that bad.
Treating vein problems early, when your main symptom is just leg heaviness and fatigue, is easier and more effective than waiting until you have advanced vein disease. You'll feel better faster, prevent complications, and improve your quality of life.
Your legs carry you through every day of your life. They deserve to feel light, energetic, and comfortable. If they're telling you something's wrong, it's worth listening.
FAQs About Heavy and Tired Legs
Is leg heaviness always caused by vein problems?
Not always, but venous insufficiency is one of the most common causes, especially if the heaviness follows a pattern of worsening throughout the day and improving with elevation. Other potential causes include muscle fatigue, joint problems, medication side effects, or other circulation issues. A proper evaluation can determine the exact cause of your symptoms.
Can dehydration make my legs feel heavy?
Yes, dehydration can contribute to leg heaviness because it makes your blood thicker and more difficult to pump. However, if you're well-hydrated and still experiencing persistent leg heaviness, especially with the typical end-of-day worsening pattern, vein problems are a more likely culprit.
Why do my legs feel heavier in hot weather?
Heat causes your veins to dilate (expand), which can worsen blood pooling if you have underlying venous insufficiency. Many people with vein problems notice their symptoms are worse during summer months or after hot baths. Keeping your legs cool and avoiding prolonged heat exposure can help.
Will losing weight make my legs feel less heavy?
If you're carrying extra weight, losing pounds can significantly reduce pressure on your leg veins and improve symptoms. However, if you have damaged vein valves, weight loss alone may not completely resolve the problem. It's still worth pursuing as part of an overall approach to better vein health.
How long does leg heaviness last after standing all day?
With healthy veins, any leg tiredness from prolonged standing should resolve within an hour or so of resting or elevating your legs. If the heavy feeling persists for hours or doesn't significantly improve with rest and elevation, it suggests an underlying vein problem rather than just normal muscle fatigue.
Can exercise make heavy legs worse?
Exercise generally improves circulation and helps with venous fatigue, but high-impact activities or heavy weightlifting can temporarily increase symptoms. Low-impact exercises like walking, swimming, and cycling are best for people with vein problems. If exercise consistently makes your leg heaviness worse, talk to a vein specialist.
Are compression socks a permanent solution for heavy legs?
Compression stockings can provide excellent symptom relief and are a great management tool, but they're treating the symptom, not the underlying cause. They work as long as you're wearing them, but they won't fix damaged vein valves. Many people use compression stockings while exploring treatment options or as ongoing support after treatment.
Do I need to see a vein specialist or can my regular doctor help?
Your regular doctor can perform an initial evaluation and may suggest conservative measures. However, a vein specialist has focused expertise in diagnosing and treating venous conditions. If your symptoms persist despite conservative management, or if you want to explore treatment options, seeing a specialist like Dr. Sorace is recommended.
FAQs About The Vein Institute
What happens during a vein evaluation?
Your evaluation will include a consultation about your symptoms and medical history, a physical examination of your legs, and typically a painless venous ultrasound to assess how blood is flowing through your veins. The ultrasound shows Dr. Sorace exactly which veins aren't functioning properly and helps guide treatment recommendations.
How long does an appointment take?
Plan for about an hour for your initial consultation and evaluation. This allows time for a thorough discussion of your symptoms, physical examination, and ultrasound imaging if needed.
Will my insurance cover evaluation and treatment?
Most insurance plans cover vein evaluation and treatment when symptoms like leg heaviness, swelling, and pain indicate a medical problem rather than just a cosmetic concern. Our team will verify your insurance benefits and explain your coverage before you proceed with any treatment.
Can I be treated the same day as my consultation?
Treatment planning depends on your specific condition and insurance requirements. While same-day treatment may be possible in some cases, most patients prefer to schedule treatment for a separate visit after they've had time to discuss options and prepare.
Where is The Vein Institute located?
We have two convenient locations in Texas. Our San Antonio clinic is at 14530 NW Military Hwy, Suite 100, San Antonio, TX 78231. Our Boerne office is at 745 West San Antonio Ave, Suite 100, Boerne, TX 78006. Both locations offer comprehensive vein care.
How do I schedule an appointment?
Call our San Antonio office at (210) 236-9372 or our Boerne office at (830) 331-9900 to schedule your consultation. You can also visit our contact page to request an appointment online.
Ready to find out why your legs feel heavy and tired? Contact The Vein Institute today to schedule your evaluation with Dr. Sorace.
San Antonio Office: 14530 NW Military Hwy, Suite 100, San Antonio, TX 78231 | Phone: (210) 236-9372
Boerne Office: 745 West San Antonio Ave, Suite 100, Boerne, TX 78006 | Phone: (830) 331-9900
Your legs don't have to feel heavy anymore. Let's find out what's going on and get you back to feeling comfortable and energetic.
Disclaimer: The information provided on this blog is for general informational purposes only and is not intended as, and should not be considered, medical advice. All information, content, and material available on this blog are for general informational purposes only. Readers are advised to consult with a qualified healthcare professional for medical advice, diagnosis, or treatment. The author and the blog disclaim any liability for the decisions you make based on the information provided. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.