Why Are My Legs and Ankles Swollen? When Swelling Could Be a Vein Problem
Key Points
- Leg and ankle swelling that worsens throughout the day often indicates venous insufficiency
- Swelling from vein problems typically affects both legs and improves with elevation
- Chronic swelling can lead to skin changes and more serious complications if left untreated
- One-sided sudden swelling requires immediate medical attention as it may signal a blood clot
- Compression stockings and lifestyle changes can help manage swelling but won't fix underlying vein disease
- Early evaluation and treatment prevent swelling from progressing to permanent tissue damage
- Most vein-related swelling is treatable with minimally invasive procedures
You kick off your shoes at the end of the day and notice your ankles look puffy. Your socks leave deep indentations on your legs. Your feet feel tight and uncomfortable, like they're stuffed into shoes that suddenly don't fit right. Maybe the swelling goes away overnight, or maybe it's becoming more constant.
Swollen legs and ankles are incredibly common, but that doesn't mean they're normal or something you should just accept. In many cases, persistent leg swelling is your body's way of waving a red flag that your veins aren't working the way they should.
Let's talk about why swelling happens, when it's related to vein problems, and what you can do about it.
What Does Vein-Related Swelling Look Like?
Before we dive into causes, let's make sure we're talking about the same kind of swelling. Vein-related leg swelling has some distinctive characteristics that help differentiate it from other types of swelling.
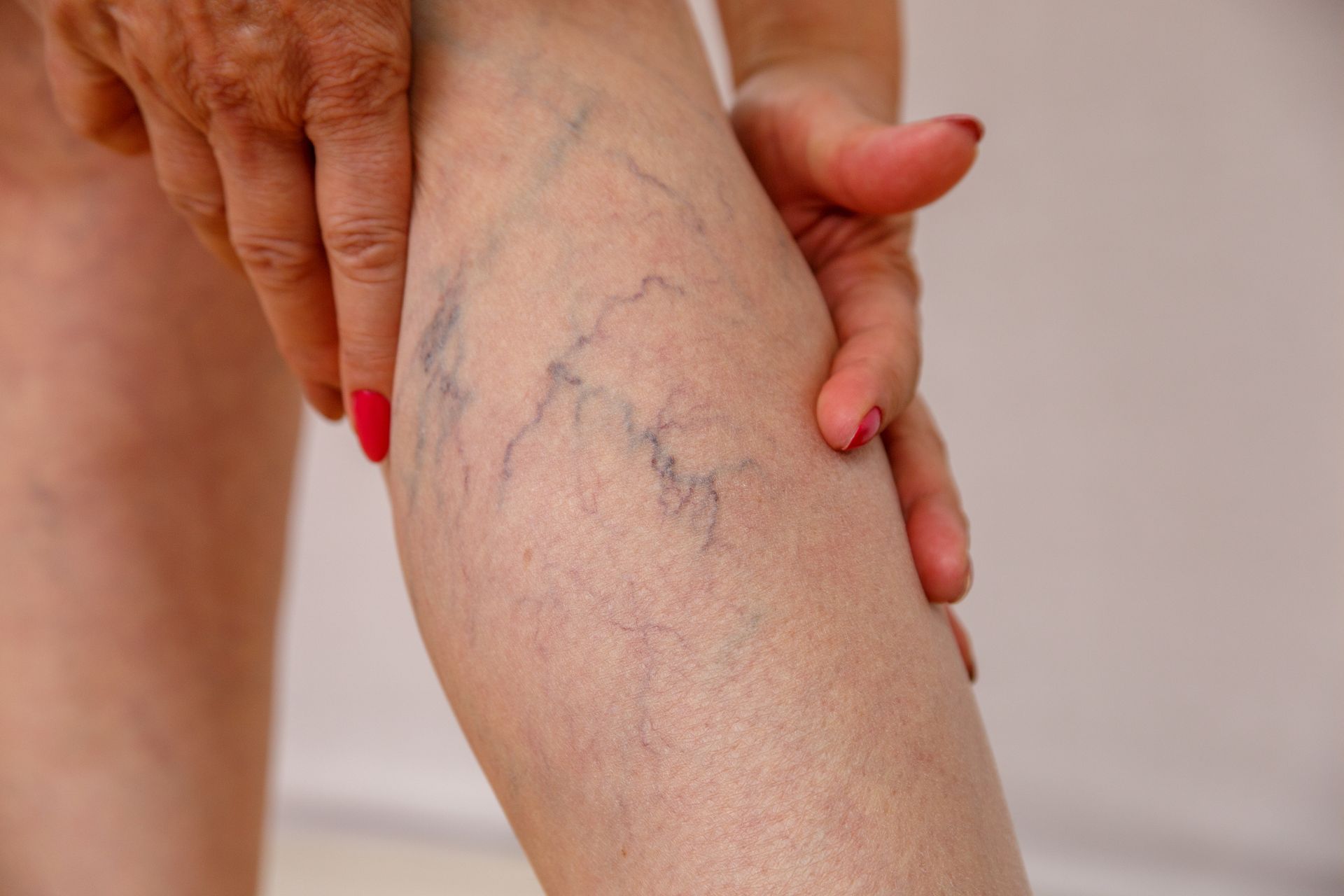
Location matters: Swelling from vein problems typically starts at your ankles and can extend up into your calves and lower legs. It usually affects the lower part of your legs more than the upper part. Your feet might swell too, making your shoes feel uncomfortably tight by the end of the day.
The pattern is predictable: This is one of the biggest clues. Vein-related swelling follows a consistent daily pattern. You wake up with relatively normal-looking legs and ankles. As the day progresses and you're upright (standing or sitting), the swelling gradually builds. By evening, your ankles are noticeably puffy. After a night of sleep with your legs elevated, the swelling improves or goes away completely, only to return again the next day.
It's often bilateral: Swelling from venous insufficiency usually affects both legs, though one side might be worse than the other. If you have sudden swelling in only one leg, that's a different situation that needs immediate medical attention (more on that later).
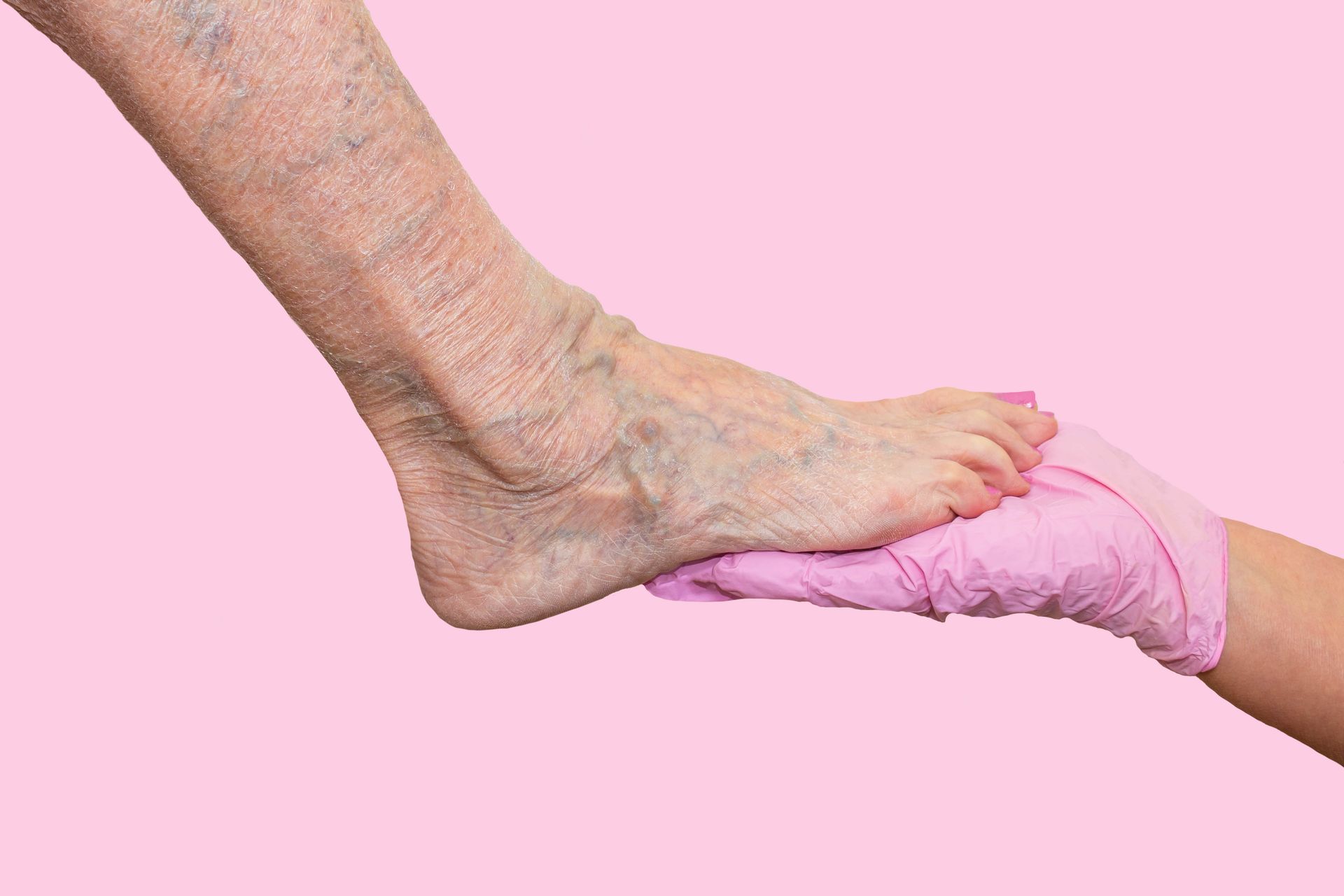
The pitting test: If you press your finger into the swollen area and it leaves an indentation that takes a few seconds to bounce back, that's called "pitting edema." This is typical of vein-related swelling.
Associated symptoms: Vein swelling rarely shows up alone. You'll often notice other signs like leg heaviness, achiness, visible veins, or skin changes. If you've been experiencing that heavy, tired feeling in your legs, swelling might be the next symptom to develop.
Why Veins Cause Swelling: The Simple Explanation
To understand why bad veins lead to swollen legs, you need to know a little about how your circulatory system is supposed to work.
Your leg veins are responsible for moving blood back up to your heart against gravity. Inside these veins are tiny one-way valves that open to let blood flow upward and close to prevent it from flowing backward. Your calf muscles act like a pump, squeezing the veins with each step and pushing blood up through those valves.
When this system works properly, blood circulates efficiently and fluid stays balanced in your tissues.
But when you have venous insufficiency, those valves become weak or damaged and can't close completely. Blood leaks backward and pools in your lower legs. This creates increased pressure inside your veins, kind of like water pressure building up in a hose.
That increased pressure forces fluid out of your blood vessels and into the surrounding tissues. This leaked fluid is what causes the visible swelling in your legs and ankles. The longer you're upright, the more blood pools in your legs, the higher the pressure gets, and the more fluid leaks out into your tissues.
When you lie down at night and elevate your legs, gravity finally works in your favor. The pooled blood can drain back toward your heart, the pressure decreases, and the leaked fluid gets reabsorbed. That's why your swelling improves overnight.
This explanation is a bit simplified, but it captures the basic mechanism. Your veins aren't moving blood efficiently, pressure builds up, and fluid leaks out. The result? Swollen, uncomfortable legs and ankles.
The Daily Pattern: Why Swelling Gets Worse Throughout the Day
If you have vein-related swelling, you've probably noticed it follows a frustratingly predictable schedule. Understanding why this happens can actually be reassuring because it confirms that your veins are the likely culprit.
Morning: You wake up and your legs look pretty normal. After lying flat all night with your legs at heart level, most of the pooled blood has drained back up. The fluid that leaked into your tissues overnight has been reabsorbed. Your veins got a break from fighting gravity for 7-8 hours, and it shows.
Mid-morning to early afternoon: As you go about your day, gravity starts working against your veins. If you have weak vein valves, blood begins pooling in your lower legs almost immediately when you stand up. But early in the day, the accumulation is still minimal. You might not notice any swelling yet, though your legs might start feeling a bit heavier.
Late afternoon: By now, you've been upright for hours. More and more blood has pooled in your leg veins. The pressure has been building steadily. Fluid has been slowly leaking into your tissues. You start to notice your ankles looking puffier than they did this morning. Your shoes might feel a bit snug.
Evening: This is when swelling typically peaks. You've accumulated hours of blood pooling and fluid buildup. Your ankles might be noticeably swollen. Sock marks are deep and take a while to fade. Your legs feel heavy and tight. Some people describe their legs as feeling "full" or "stuffed."
Nighttime: When you finally get to elevate your legs and lie down, relief starts almost immediately. You can literally feel your legs "draining." The swelling gradually decreases overnight, preparing to start the whole cycle again tomorrow.
This daily reset-and-worsen pattern is a hallmark of vein-related swelling. Other types of swelling (from heart problems, kidney issues, or lymphedema) don't typically improve overnight the way vein swelling does.
When Swelling Signals Venous Insufficiency
Not all leg swelling comes from vein problems, but certain characteristics make venous insufficiency the likely cause.
The swelling is chronic and progressive: If you've been dealing with leg swelling for weeks or months, and it seems to be getting gradually worse over time, venous insufficiency is a strong possibility.
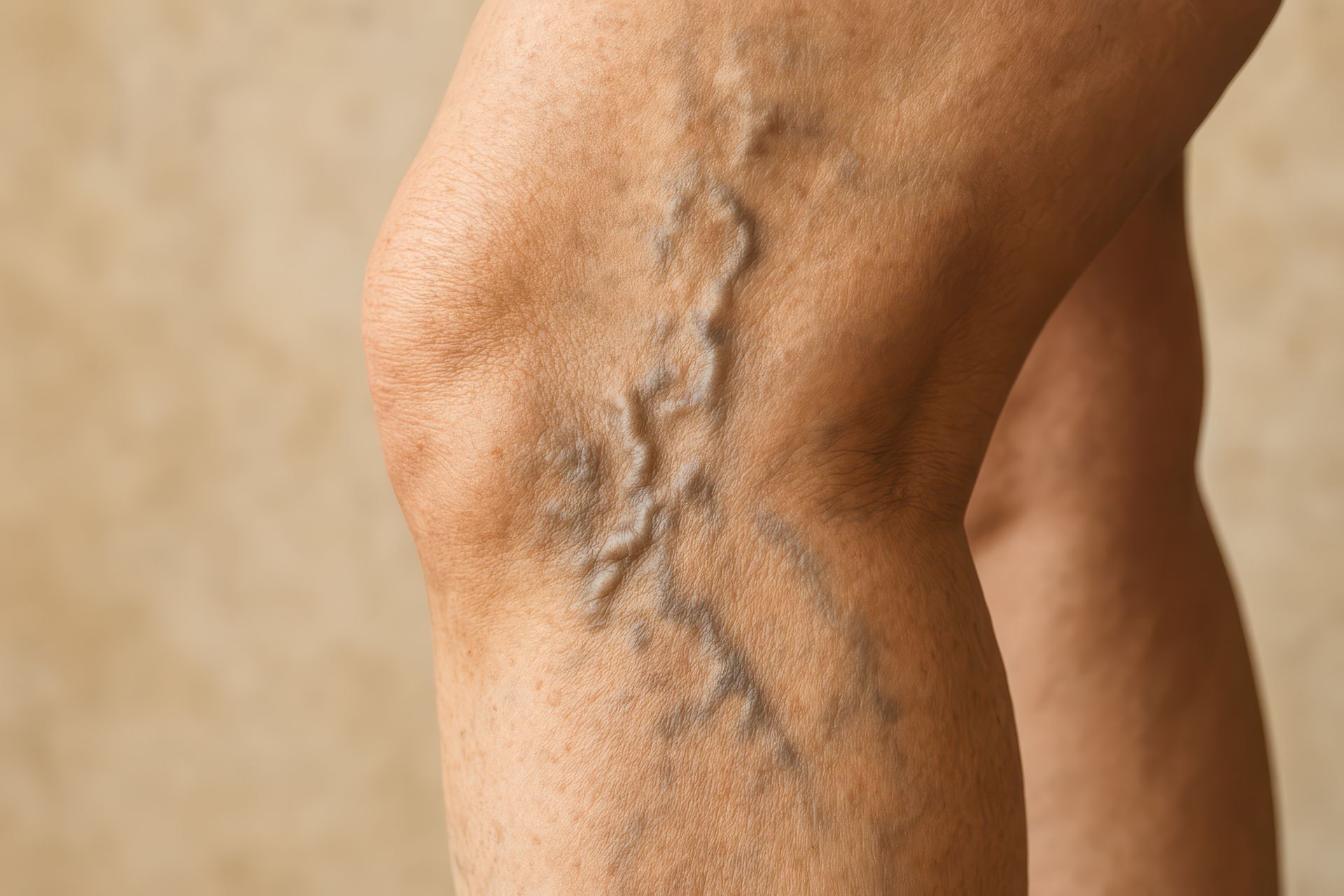
You have other vein symptoms: Swelling combined with leg heaviness, visible varicose veins, aching, nighttime cramping, or restless legs suggests your veins are struggling. These symptoms rarely travel alone.
The swelling follows the daily pattern: That morning-to-evening worsening cycle with overnight improvement is classic for venous insufficiency.
Elevation helps significantly: If propping your feet up provides noticeable relief and reduces swelling, that tells you gravity and blood pooling are major factors.
You have risk factors: If you stand or sit all day for work, you're overweight, you've been pregnant, or you have a family history of vein problems, these increase the likelihood that your swelling is vein-related.
Skin changes are developing: Over time, chronic venous insufficiency can cause skin discoloration (usually brownish patches near your ankles), thickening of the skin, or a shiny, tight appearance. These changes indicate that swelling has been present long enough to affect your skin.
If several of these characteristics match your situation, there's a good chance you're dealing with venous insufficiency. The comprehensive guide on vein problems can help you understand how these symptoms fit together.
Other Causes of Leg Swelling (Not Vein-Related)
While this blog focuses on vein-related swelling, it's important to know that other conditions can cause similar symptoms. Here are some other common causes:
Medications: Certain blood pressure medications, steroids, antidepressants, and diabetes medications can cause leg swelling as a side effect.
Heart problems: When your heart isn't pumping efficiently, fluid can back up into your legs. Heart-related swelling usually affects both legs equally and may be accompanied by shortness of breath.
Kidney disease: Your kidneys help regulate fluid balance. When they're not working properly, fluid can accumulate throughout your body, including your legs.
Liver disease: Severe liver problems can cause fluid retention and leg swelling along with other symptoms like abdominal swelling.
Lymphedema: This occurs when your lymphatic system can't properly drain fluid. It tends to cause more severe, chronic swelling that doesn't improve much with elevation.
Injury or infection: A sprained ankle, broken bone, or infection can cause localized swelling in one leg.
Prolonged sitting: Long flights or car rides can cause temporary swelling in anyone, even people with healthy veins.
Pregnancy: Hormonal changes and pressure from the growing uterus commonly cause leg swelling during pregnancy.
A vein specialist can help determine whether your swelling is from venous insufficiency or another cause. Sometimes multiple factors contribute to swelling, and sorting it out requires professional evaluation.
When Swelling Is an Emergency: The Blood Clot Warning
Most leg swelling develops gradually and isn't dangerous, but there's one situation that requires immediate medical attention: sudden swelling in one leg that could signal a blood clot (deep vein thrombosis or DVT).
Go to the emergency room or call 911 if you experience:
- Sudden swelling in one leg (not both)
- Pain, warmth, and redness in the swollen leg
- The swollen leg feels significantly warmer than the other leg
- Firm or hard areas in the swollen leg
- Shortness of breath or chest pain (could indicate the clot has traveled to your lungs)
Blood clots are serious and potentially life-threatening. They require immediate treatment. Don't wait to see if it gets better on its own.
The gradual, bilateral swelling from venous insufficiency is a chronic condition, not an emergency. But sudden, one-sided swelling with the characteristics above is completely different and needs urgent evaluation.
How Swelling Progresses When Left Untreated
Here's something important to understand: vein-related swelling doesn't stay the same. It's progressive, meaning it gets worse over time if you don't address the underlying vein problem.
Early stage: Swelling is mild and only noticeable by late afternoon or evening. It completely resolves overnight. You might barely notice it or think it's just normal end-of-day tiredness.
Moderate stage: Swelling becomes more pronounced and starts earlier in the day. It takes longer to resolve at night. You need to actively elevate your legs to get relief. Your shoes definitely feel tight by evening. Other symptoms like leg heaviness and aching become more bothersome.
Advanced stage: Swelling is present most of the time, even in the morning. It doesn't completely resolve overnight anymore. Your skin starts showing changes like discoloration, thickening, or a shiny, tight appearance. You might develop skin irritation or itching.
Severe stage: Chronic, severe swelling can lead to skin breakdown and venous ulcers (open sores that won't heal). Once you reach this stage, treatment becomes more complicated and recovery takes longer.
The good news? You don't have to wait until you reach advanced stages to get help. Treating venous insufficiency early, when swelling is still mild or moderate, is much easier and more effective. You can prevent progression and avoid serious complications.
What You Can Do About Swelling Right Now
While you're deciding whether to see a specialist or waiting for your appointment, there are several strategies that can help reduce swelling and improve your comfort.
Elevate your legs regularly: Prop your feet up above heart level for 15-20 minutes several times throughout the day. This is one of the most effective ways to reduce swelling quickly.
Move more: Whether you sit or stand all day, make a point to move around regularly. Walking activates your calf muscle pump and helps move blood upward. Even simple ankle circles and calf raises while sitting can help.
Try compression stockings: These provide graduated pressure that helps push blood back toward your heart and prevents fluid from accumulating in your tissues. You can buy over-the-counter compression socks or get a prescription for stronger medical-grade stockings.
Reduce salt intake: Excess sodium causes your body to retain water, which can worsen swelling. Pay attention to processed foods, which tend to be very high in salt.
Stay hydrated: It seems counterintuitive, but drinking plenty of water actually helps reduce swelling by preventing your body from holding onto excess fluid.
Lose weight if needed: Extra body weight puts additional pressure on your leg veins. Even modest weight loss can reduce swelling.
Avoid sitting with your legs down for long periods: If you have a desk job, try to prop your feet up on a small stool or box rather than letting them hang down all day.
Don't cross your legs: This position restricts circulation and can worsen blood pooling.
Exercise regularly: Low-impact activities like walking, swimming, and cycling are excellent for improving circulation without putting excessive stress on your veins.
These conservative measures can provide relief and may slow the progression of vein problems, but they won't fix damaged vein valves or cure venous insufficiency. For more detailed advice, check out our post on daily habits that improve circulation and reduce vein symptoms.
How Compression Stockings Help (And Their Limitations)
Compression stockings deserve special mention because they're often the first line of defense against vein-related swelling.
These aren't your regular athletic socks or casual compression socks. Medical-grade compression stockings are specifically designed with graduated compression, meaning they're tightest at the ankle and gradually decrease in pressure as they go up your leg. This design helps push blood upward against gravity.
How they help:
- Reduce the amount of blood pooling in your lower legs
- Decrease the pressure that forces fluid into your tissues
- Prevent swelling from developing or worsening during the day
- Provide support to stretched vein walls
- Improve overall circulation in your legs
Many people get significant relief from compression stockings. Your legs feel less heavy and tired, and swelling is noticeably reduced when you wear them consistently.
But here's the limitation: Compression stockings are a management tool, not a cure. They work while you're wearing them, but they're not fixing the underlying problem with your vein valves. The damaged valves are still damaged. The venous insufficiency is still there.
Think of compression stockings like glasses for your eyes. They help you see better when you're wearing them, but they don't cure your vision problem. Similarly, compression stockings help reduce swelling while you wear them, but they don't cure venous insufficiency.
That said, they're incredibly useful for managing symptoms, especially if you're not ready for treatment, if you need to delay treatment for any reason, or as ongoing support after treatment.
When to See a Vein Specialist About Swelling
You don't need to suffer through months or years of progressive leg swelling before seeking help. Here are signs that it's time to see a specialist:
Your swelling is persistent: If you've had leg swelling for more than a few weeks and it's not going away, get it evaluated.
The swelling is getting worse: Progressive worsening over weeks or months suggests an underlying problem that needs treatment.
Conservative measures aren't helping: If you've tried compression stockings, elevation, exercise, and lifestyle changes without much improvement, it's time to explore other options.
You're developing skin changes: Discoloration, thickening, or any changes to your skin texture indicate that swelling has progressed to a more serious stage.
The swelling affects your daily life: If swelling limits your activities, makes it hard to find comfortable shoes, keeps you from exercising, or bothers you enough that you think about it regularly, that's reason enough to get help.
You have other vein symptoms: Swelling combined with visible varicose veins, leg heaviness, aching, or cramping strongly suggests venous insufficiency that would benefit from treatment.
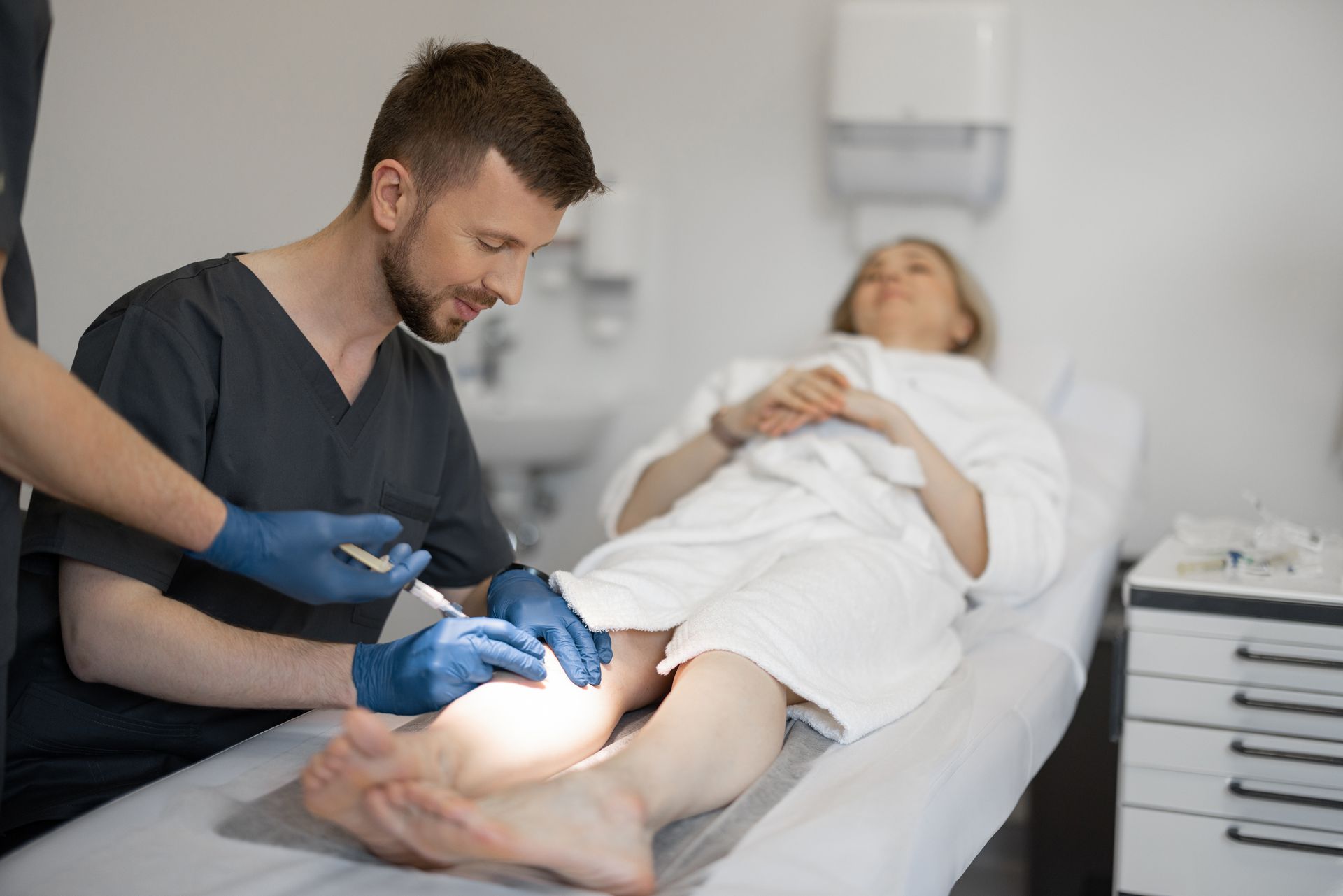
Dr. Michael Sorace can perform a simple, painless ultrasound to assess your vein function and determine the cause of your swelling. Early diagnosis gives you more treatment options and better outcomes.
What Treatment Can Do for Swollen Legs
Here's the encouraging part: when swelling is caused by venous insufficiency, treatment can be remarkably effective.
By addressing the underlying vein problem, blood can flow efficiently again. The pooling stops. The pressure decreases. Fluid stops leaking into your tissues. Your legs can drain properly, and the chronic swelling finally resolves.
Most patients notice significant improvement in swelling within weeks of treatment. Your ankles look normal again. Your shoes fit comfortably all day. That tight, full feeling in your legs goes away. You don't need to elevate your legs constantly just to feel comfortable.
Modern vein treatments are minimally invasive, performed in the office, and have excellent success rates for reducing swelling and other symptoms of venous insufficiency. Recovery is quick, and most people return to normal activities within a day or two.
The Vein Institute specializes in diagnosing and treating the vein problems that cause chronic leg swelling. The first step is understanding exactly what's happening with your veins and creating a personalized treatment plan.
Living with Chronic Swelling Takes a Toll
Beyond the physical discomfort, chronic leg swelling affects your life in ways that other people might not understand.
You avoid wearing certain clothes because your swollen ankles are visible. Shopping for shoes becomes frustrating because your feet are different sizes in the morning versus the evening. You feel self-conscious at the pool or beach. You're constantly adjusting your position, trying to find relief.
The tiredness and heaviness make it harder to stay active. You start declining invitations because you know your legs will hurt. You plan your day around when and where you can elevate your legs.
This isn't just about vanity or minor inconvenience. Chronic swelling genuinely impacts your quality of life and your physical health. You deserve legs that feel comfortable and function normally.
The good news is that help is available, and treatment really works. You don't have to accept swollen legs as your new normal.
FAQs About Swollen Legs and Ankles
Is it normal for my legs to swell after sitting all day?
Some mild swelling after prolonged sitting is common for everyone, but if the swelling is significant, happens daily, and doesn't quickly resolve when you start moving around, it suggests an underlying vein problem rather than just normal temporary swelling.
Why does only one ankle swell sometimes?
If you consistently have more swelling in one leg than the other, it usually means the vein problem is worse on that side. However, sudden swelling in only one leg with pain and warmth could indicate a blood clot and requires immediate medical attention.
Can drinking more water reduce leg swelling?
Yes, staying well-hydrated can actually help reduce swelling. When you're dehydrated, your body holds onto fluid, which can worsen swelling. Drinking adequate water helps your body maintain proper fluid balance.
Will losing weight get rid of my leg swelling?
Weight loss can significantly reduce leg swelling by decreasing pressure on your veins. However, if you have damaged vein valves from venous insufficiency, losing weight alone may not completely eliminate swelling. It's still worth pursuing as part of an overall approach to vein health.
How tight should compression stockings feel?
Compression stockings should feel snug but not painful. They should be tightest at your ankle and gradually looser as they go up your leg. If they're leaving deep marks, causing pain, or making your toes tingle or turn blue, they're too tight. A vein specialist can help you get the right fit.
Is leg swelling a sign of heart failure?
Leg swelling can be a symptom of heart problems, especially if it's accompanied by shortness of breath, rapid weight gain, or swelling in other parts of your body. However, venous insufficiency is a much more common cause of chronic leg swelling. A proper evaluation can determine the cause.
Can I fly with swollen legs?
You can fly, but prolonged sitting during flights can worsen swelling. Wear compression stockings during travel, walk around the cabin regularly, do ankle exercises in your seat, and stay well-hydrated. If you have a history of blood clots, talk to your doctor before flying.
How long does it take for swelling to go away after vein treatment?
Most patients notice significant improvement in swelling within 2-4 weeks after treating their vein problems. Some improvement may be noticeable within days. The timeline varies depending on how severe your swelling was and how long you've had venous insufficiency.
FAQs About The Vein Institute
What tests will you do to diagnose the cause of my swelling?
Dr. Sorace will start with a thorough discussion of your symptoms and medical history, followed by a physical examination. He'll typically perform a venous ultrasound, which is a painless test that shows how blood is flowing through your veins and whether your vein valves are working properly. This helps determine if venous insufficiency is causing your swelling.
Do you treat swelling caused by lymphedema or other non-vein conditions?
The Vein Institute specializes in vein-related conditions. If your evaluation reveals that your swelling is caused by something other than venous insufficiency, Dr. Sorace can refer you to an appropriate specialist for that condition.
How much does vein treatment cost if I don't have insurance?
Treatment costs vary depending on the specific procedures needed. Our team can provide cost estimates and discuss payment options during your consultation. Many patients are surprised to learn that insurance often covers treatment for medically necessary vein conditions.
Can I get treatment if I'm pregnant?
Generally, vein treatment is postponed until after pregnancy and breastfeeding because many pregnancy-related vein issues improve on their own after delivery. However, conservative management like compression stockings can help with symptoms during pregnancy. We're happy to evaluate you and provide guidance.
Where is The Vein Institute located?
We have two convenient Texas locations. Our San Antonio clinic is at 14530 NW Military Hwy, Suite 100, San Antonio, TX 78231. Our Boerne office is at 745 West San Antonio Ave, Suite 100, Boerne, TX 78006. Both offices offer comprehensive vein evaluations and treatment.
How do I schedule an appointment?
Call our San Antonio office at (210) 236-9372 or our Boerne office at (830) 331-9900 to schedule your consultation. You can also visit our contact page to request an appointment online.
Ready to find out what's causing your leg and ankle swelling? Contact The Vein Institute today to schedule your evaluation with Dr. Sorace.
San Antonio Office: 14530 NW Military Hwy, Suite 100, San Antonio, TX 78231 | Phone: (210) 236-9372
Boerne Office: 745 West San Antonio Ave, Suite 100, Boerne, TX 78006 | Phone: (830) 331-9900
You don't have to live with swollen, uncomfortable legs. Let's figure out what's going on and get you feeling better.
Disclaimer: The information provided on this blog is for general informational purposes only and is not intended as, and should not be considered, medical advice. All information, content, and material available on this blog are for general informational purposes only. Readers are advised to consult with a qualified healthcare professional for medical advice, diagnosis, or treatment. The author and the blog disclaim any liability for the decisions you make based on the information provided. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.